STOMACH ANATOMY I
Gray's Anatomy 39th
The stomach is the widest part of the alimentary tract and lies between the oesophagus and the duodenum. It is situated in the upper abdomen, extending from the left upper quadrant downwards, forwards and to the right, lying in the left hypochondriac, epigastric and umbilical areas. It occupies a recess beneath the diaphragm and anterior abdominal wall that is bounded by the upper abdominal viscera on either side. Its mean capacity increases from c.30 ml at birth, to 1000 ml at puberty, to c.1500 ml in adults. The peritoneal surface of the stomach is interrupted by the attachments of the greater and lesser omenta, which define the greater and lesser curvatures separating two surfaces
The stomach is the widest part of the alimentary tract and lies between the oesophagus and the duodenum. It is situated in the upper abdomen, extending from the left upper quadrant downwards, forwards and to the right, lying in the left hypochondriac, epigastric and umbilical areas. It occupies a recess beneath the diaphragm and anterior abdominal wall that is bounded by the upper abdominal viscera on either side. Its mean capacity increases from c.30 ml at birth, to 1000 ml at puberty, to c.1500 ml in adults. The peritoneal surface of the stomach is interrupted by the attachments of the greater and lesser omenta, which define the greater and lesser curvatures separating two surfaces
PARTS OF THE STOMACH
The stomach is divided for descriptive purposes into the fundus, body, pyloric antrum and pylorus, by arbitrary lines drawn on its external surface. The internal appearance and microstructure of these regions varies to some degree. The fundus is dome shaped and projects above and to the left of the cardiac orifice to lie in contact with the left dome of the diaphragm. It lies above a line drawn horizontally from the incisura cardiaca to the greater curvature. The body extends from the fundus to the incisura angularis, which is a constant external notch at the lower end of the lesser curvature. A line drawn from the incisura angularis to an indentation on the greater curvature defines the lower boundary of the body. The pyloric antrum extends from this line to the sulcus intermedius. At this point, the stomach narrows to become the pyloric canal, which is usually only 1-2 cm in length and terminates at the pyloric orifice.
GASTRIC RELATIONS
GASTRIC CURVATURES
Lesser curvature
The lesser curvature extends between the cardiac and pyloric orifices and forms the medial (posterior and superior) border of the stomach. It descends from the medial side of the oesophagus in front of the decussating fibres of the right crus of the diaphragm. It curves downwards and to the right and lies anterior to the superior border of the pancreas. It ends at the pylorus just to the right of the midline. In the most dependent part there is typically a notch, the incisura angularis, whose position and appearance vary with gastric distension. The lesser omentum is attached to the lesser curvature and contains the right and left gastric vessels.
Greater curvature
The greater curvature is four or five times longer than the lesser. It starts from the incisura cardiaca formed between the lateral border of the abdominal oesophagus and the fundus of the stomach. It arches upwards, posterolaterally and to the left. Its highest convexity, the apex of the fundus, is approximately level with the left fifth intercostal space just below the left nipple in males, but varies with respiration. From this level it sweeps inferiorly and anteriorly, slightly convex to the left, almost as far as the tenth costal cartilage in the supine position, where it turns medially to end at the pylorus. There is frequently a groove, termed the sulcus intermedius, in the curvature close to the pyloric constriction. The start of the greater curvature is covered by peritoneum, which continues over the anterior surface of the stomach. Laterally the greater curvature gives attachment to the gastrosplenic ligament and beyond this to the greater omentum, which contains the gastroepiploic vessels. The gastrosplenic ligament and the greater omentum, together with the gastrophrenic and splenorenal ligaments, are continuous parts of the original dorsal mesogastrium. The names merely indicate regions of the same continuous sheet of peritoneum and associated connective tissue.
Gastric volvulus
Volvulus of the stomach is much less common than volvulus of either the sigmoid colon or caecum. Two types of gastric volvulus may occur. The first, organoaxial volvulus, occurs about a line of rotation running from below the cardiac orifice to the pylorus. The antrum, body and fundus rotate upwards, with the greater curvature coming to lie above the lesser curvature as the volvulus progresses. The second, mesenteroaxial volvulus, occurs about a line drawn 'across' the body of the stomach, usually just above the incisura angularis. This type of volvulus is perpendicular to the line of organoaxial volvulus. The distal body and antrum rotate anteriorly, superiorly and laterally whilst the upper body and fundus rotate posteriorly, medially and inferiorly. Although relatively mobile within the upper abdomen, the stomach is normally tethered to the oesophagus at the gastro-oesophageal junction, to the duodenum at the pylorus, to the spleen by the gastrosplenic omentum, and to the liver by the lesser omentum. The attachment to the transverse colon via the gastrocolic omentum also restrains the stomach but is the most mobile of all. For either type of gastric volvulus to occur, it is necessary for some or all of these points of tethering to be loosened either by previous surgical division or by chronic lengthening and loosening of their connective tissue. Organoaxial volvulus is most common because the lesser omentum, gastrosplenic ligament and gastrocolic omentum are more likely to undergo chronic lengthening by traction than the other attachments of the stomach. Mesenteroaxial volvulus requires the gastro-oesophageal junction and pylorus to be sufficiently mobile as to come into close approximation. These structures are firmly tethered and consequently this form of gastric volvulus is much less common. Despite the profuse gastric arterial supply, either type of volvulus may compromise the vascularity of the stomach.
GASTRIC SURFACES
When the stomach is empty and contracted, the two surfaces tend to lie facing almost superiorly and inferiorly, but with increasing degrees of distension they come to face progressively more anteriorly and posteriorly.
Anterior (superior) surface
The lateral part of the anterior surface is posterior to the left costal margin and in contact with the diaphragm, which separates it from the left pleura, the base of the left lung, the pericardium and the left sixth to ninth ribs (Fig. 2). It lies posterior to the costal attachments of the upper fibres of transversus abdominis, which separate it from the seventh to ninth costal cartilages. The upper and left part of this surface curves posterolaterally and is in contact with the gastric surface of the spleen. The right half of the anterior surface is related to the left and quadrate lobes of the liver and the anterior abdominal wall. When the stomach is empty, the transverse colon may lie adjacent to the anterior surface. The entire anterior (superior) surface is covered by peritoneum.
Gastric volvulus
Volvulus of the stomach is much less common than volvulus of either the sigmoid colon or caecum. Two types of gastric volvulus may occur. The first, organoaxial volvulus, occurs about a line of rotation running from below the cardiac orifice to the pylorus. The antrum, body and fundus rotate upwards, with the greater curvature coming to lie above the lesser curvature as the volvulus progresses. The second, mesenteroaxial volvulus, occurs about a line drawn 'across' the body of the stomach, usually just above the incisura angularis. This type of volvulus is perpendicular to the line of organoaxial volvulus. The distal body and antrum rotate anteriorly, superiorly and laterally whilst the upper body and fundus rotate posteriorly, medially and inferiorly. Although relatively mobile within the upper abdomen, the stomach is normally tethered to the oesophagus at the gastro-oesophageal junction, to the duodenum at the pylorus, to the spleen by the gastrosplenic omentum, and to the liver by the lesser omentum. The attachment to the transverse colon via the gastrocolic omentum also restrains the stomach but is the most mobile of all. For either type of gastric volvulus to occur, it is necessary for some or all of these points of tethering to be loosened either by previous surgical division or by chronic lengthening and loosening of their connective tissue. Organoaxial volvulus is most common because the lesser omentum, gastrosplenic ligament and gastrocolic omentum are more likely to undergo chronic lengthening by traction than the other attachments of the stomach. Mesenteroaxial volvulus requires the gastro-oesophageal junction and pylorus to be sufficiently mobile as to come into close approximation. These structures are firmly tethered and consequently this form of gastric volvulus is much less common. Despite the profuse gastric arterial supply, either type of volvulus may compromise the vascularity of the stomach.
GASTRIC SURFACES
When the stomach is empty and contracted, the two surfaces tend to lie facing almost superiorly and inferiorly, but with increasing degrees of distension they come to face progressively more anteriorly and posteriorly.
Anterior (superior) surface
The lateral part of the anterior surface is posterior to the left costal margin and in contact with the diaphragm, which separates it from the left pleura, the base of the left lung, the pericardium and the left sixth to ninth ribs (Fig. 2). It lies posterior to the costal attachments of the upper fibres of transversus abdominis, which separate it from the seventh to ninth costal cartilages. The upper and left part of this surface curves posterolaterally and is in contact with the gastric surface of the spleen. The right half of the anterior surface is related to the left and quadrate lobes of the liver and the anterior abdominal wall. When the stomach is empty, the transverse colon may lie adjacent to the anterior surface. The entire anterior (superior) surface is covered by peritoneum.
Posterior (inferior) surface
The posterior surface lies anterior to the left crus and lower fibres of the diaphragm, the left inferior phrenic vessels, the left suprarenal gland, the superior pole of the left kidney, the splenic artery, the anterior pancreatic surface, the splenic flexure of the colon and the upper layer of the transverse mesocolon (Fig. 3). Together these form the shallow stomach bed: they are separated from the stomach by the lesser sac (over which the stomach slides as it distends). The upper left part of the surface curves anterolaterally and lies in contact with the gastric surface of the spleen. The greater omentum and the transverse mesocolon separate the stomach from the duodenojejunal flexure and ileum. The posterior surface is covered by peritoneum, except near the cardiac orifice, where a small, triangular area contacts the left diaphragmaticcrus and sometimes the left suprarenal gland. The left gastric vessels reach the lesser curvature at the right extremity of this bare area in the left gastropancreatic fold. The gastrophrenic ligament passes from the lateral aspect of this bare area to the inferior surface of the diaphragm.
GASTRIC ORIFICES
CARDIAC ORIFICE AND GASTRO-OESOPHAGEAL JUNCTION
The opening from the oesophagus into the stomach is the cardiac orifice (Fig. 4). It is typically situated to the left of the midline behind the seventh costal cartilage at the level of the eleventh thoracic vertebra. It is c.10 cm from the anterior abdominal wall and 40 cm from the incisor teeth. The short abdominal part of the oesophagus curves sharply to the left as it descends and is continuous with the cardiac orifice. The right side of the oesophagus is continuous with the lesser curvature, the left side with the greater curvature. There is no specific anatomical cardiac sphincter related to the orifice.
Internally, the transition between oesophagus and stomach is difficult to define because mucosa of gastric fundal pattern extends a variable distance up into the abdominal oesophagus. It usually forms a 'zig-zag' squamo-columnar epithelial junction with the oesophageal epithelium above this Z line (p. 1152). This is often referred to as the gastro-oesophageal junction, for histological and endoscopic purposes. A sling of longitudinal gastric muscle forms a loop on the superior, left, side of the gastro-oesophageal junction between the oesophagus and the lesser curvature, and this is taken as the external boundary of this junction.
Internally, the transition between oesophagus and stomach is difficult to define because mucosa of gastric fundal pattern extends a variable distance up into the abdominal oesophagus. It usually forms a 'zig-zag' squamo-columnar epithelial junction with the oesophageal epithelium above this Z line (p. 1152). This is often referred to as the gastro-oesophageal junction, for histological and endoscopic purposes. A sling of longitudinal gastric muscle forms a loop on the superior, left, side of the gastro-oesophageal junction between the oesophagus and the lesser curvature, and this is taken as the external boundary of this junction.
GASTRO-OESOPHAGEAL REFLUX
 Figure 4 The valve-like structure formed by the angle of the wall at the cardiac orifice. (Provided by Donald E Low, Department of Surgery, Virginia Mason, Seattle, USA.)
Figure 4 The valve-like structure formed by the angle of the wall at the cardiac orifice. (Provided by Donald E Low, Department of Surgery, Virginia Mason, Seattle, USA.)Reflux of gastric contents into the abdominal and lower thoracic oesophagus as a result of transient relaxation of the lower oesophageal sphincter occurs as a normal event in most individuals for a small percentage of their daily life. It also occurs as a result of a weak lower oesophageal sphincter, or of hiatus hernia which disrupts the normal anatomical barriers (p. 1083). Several anatomical and physiological factors normally prevent gastro-oesophageal reflux. The folds of gastric mucosa present in the gastro-oesophageal junction, the mucosal rosette, contribute to the formation of a fluid-and gas-tight seal. They also help to ensure that even low levels of tone within the lower oesophageal wall muscles may occlude the lumen of the junction against low pressures of gastric gas. The angle of the cardiac orifice may help to form a type of 'flap valve' and the length of abdominal oesophagus is buttressed externally by pads of adipose connective tissue at and below the level of the diaphragmatic hiatus. However, the major anti-reflux mechanism is the tonic contractions of the lower oesophageal musculature, which forms an effective high pressure zone (HPZ) (p. 986). The specialized smooth muscle of the wall of the lower oesophagus and the encircling fibres of the crural diaphragm exert a radial pressure that can be measured by a sensing device as it is withdrawn from the stomach into the oesophagus (Paterson 2001). If reflux is to be prevented, this pressure must always exceed the difference between the pressures on either side of the junction, i.e. the difference between intra-abdominal pressure (transferred to the stomach, and augmented by any contraction of the stomach wall itself), and intrathoracic pressure (transferred to the oesophagus).
During expiration, pressure exerted by tonic contraction of the smooth muscle of the lower oesophagus is normally sufficient to oppose the gastro-oesophageal pressure gradient. During inspiration, intra-abdominal pressure rises and intrathoracic pressure becomes more negative, increasing the risk of reflux. This tendency is opposed by additional pressure exerted by contraction of the crural fibres of the diaphragm. (Activation of the crural diaphragm slightly before the costal diaphragm would ensure that contraction of peri-oesophageal fibres preceded the increase in gastro-oesophageal pressure gradient.) The anti-reflux barrier must of course be lowered for swallowing and vomiting. Swallowing is followed immediately by expiration, which relaxes the crural fibres and allows the oesophageal contents to be transferred to the stomach by peristaltic movement. Vomiting is produced by bursts of activity involving co-contraction of the diaphragm, intercostal and abdominal muscles in a pattern distinct from that of respiration: this activity is coordinated with relaxation of the crural fibres around the oesophagus (Miller, 1990).
Barrett's oesophagus
The squamous epithelium lining the lower oesophagus may be pathologically replaced by a columnar, gastric type epithelium. This may occur as islands, strips, or circumferentially, and may extend for a variable length up the lower oesophagus. This process is most likely to be the result of the chronic reflux of gastric contents, acid or alkali, into the oesophagus with a resultant change in mucosal cell type. The abnormal columnar type epithelium present in the anatomical oesophagus is referred to as Barrett's epithelium.
PYLORIC ORIFICE
The pyloric orifice is the opening into the duodenum. The circular pyloric constriction on the surface of the stomach usually indicates the location of the pyloric sphincter and is often marked by a prepyloric vein crossing the anterior surface vertically downwards. The pyloric orifice typically lies 1-2 cm to the right of the midline in the transpyloric plane with the body supine and the stomach empty. The pyloric sphincter is a muscular ring formed by a marked thickening of the circular gastric muscle interlaced with some longitudinal fibres.
GASTRIC FORM AND INTERNAL APPEARANCES
To be Continued... (The Vascular, Lymphatic and Innervation)
Barrett's oesophagus
The squamous epithelium lining the lower oesophagus may be pathologically replaced by a columnar, gastric type epithelium. This may occur as islands, strips, or circumferentially, and may extend for a variable length up the lower oesophagus. This process is most likely to be the result of the chronic reflux of gastric contents, acid or alkali, into the oesophagus with a resultant change in mucosal cell type. The abnormal columnar type epithelium present in the anatomical oesophagus is referred to as Barrett's epithelium.
PYLORIC ORIFICE
The pyloric orifice is the opening into the duodenum. The circular pyloric constriction on the surface of the stomach usually indicates the location of the pyloric sphincter and is often marked by a prepyloric vein crossing the anterior surface vertically downwards. The pyloric orifice typically lies 1-2 cm to the right of the midline in the transpyloric plane with the body supine and the stomach empty. The pyloric sphincter is a muscular ring formed by a marked thickening of the circular gastric muscle interlaced with some longitudinal fibres.
GASTRIC FORM AND INTERNAL APPEARANCES
It is clear from contrast radiographic studies that the form and position of the stomach are extremely variable depending on posture, the volume of its contents, and the surrounding viscera. They are also influenced by the tone of the abdominal wall and gastric musculature and by the build of the individual. The empty stomach is most commonly J-shaped and, in the erect posture, the pylorus descends to the level of the second or the third lumbar vertebra. The lowest part of the antrum often lies below the level of the umbilicus. The fundus usually contains gas. The overall axis of the organ is, therefore, slightly inclined from the vertical (Figs 5, 6). In short, obese individuals the axis of the stomach lies more towards the horizontal as a 'steer-horn' shape.
Variation caused by the contents of the stomach mainly affects the body because the pyloric part usually remains contracted during digestion. As the stomach fills, it expands forwards and downwards but, when the colon or small bowel is distended, the fundus enlarges towards the liver and diaphragm. As stomach capacity increases, the pylorus is displaced to the right and the axis of the whole organ lies in a more oblique direction (Figs 5, 7). In this position the anterior and posterior surfaces tend to face forwards and backwards and the lowest part is the pyloric antrum, which extends below the umbilicus. When intestinal distension interferes with downward expansion of the body, the stomach retains a horizontal position.
 Figure 5 Axes of the empty and full stomach. As the stomach distends, the greater curvature 'rolls' downwards and the anterosuperior surface comes to lie almost completely vertical as the anterior surface.
Figure 5 Axes of the empty and full stomach. As the stomach distends, the greater curvature 'rolls' downwards and the anterosuperior surface comes to lie almost completely vertical as the anterior surface.
During endoscopic examination (Fig. 6), the stomach is typically at least partially distended by air. The cardiac orifice and the lowest portion of the abdominal oesophagus viewed from above are typically closed at rest by tonic contraction of the lower oesophageal musculature. The gastric mucosa lining the orifice is puckered into ridges. It is present for a short but variable distance into the abdominal oesophagus and the transition between columnar and squamous epithelium is usually clearly visible. The presence of abnormal columnar epithelium within the anatomical oesophagus is referred to as Barrett's oesophagus but the precise definition of this condition is difficult. From within the distended stomach, the cardiac orifice appears in the medial wall of the fundus and is asymmetrical. The medial edge of the cardiac orifice is continuous with the medial wall of the body of the stomach. The mucosa is slightly thickened at this point with a raised profile, forming part of the 'mucosal rosette' that lines the orifice. The 'rosette' aids closure of the cardiac orifice and helps prevent reflux of stomach contents into the oesophagus. The medial edge of the orifice is more clearly visible than the lateral edge as it forms a more acute angle with the mucosal lining of the abdominal oesophagus.
 Figure 6 Endoscopic appearance of the stomach: A, cardiac orifice from below; B, body greater curvature; C, body lesser curvature; D, pylorus.
Figure 6 Endoscopic appearance of the stomach: A, cardiac orifice from below; B, body greater curvature; C, body lesser curvature; D, pylorus.
In the partly distended stomach, the mucosa of the fundus is thrown into gentle folds with no particular pattern. As the stomach fills towards capacity, however, these folds rapidly become less pronounced, and the wall is nearly smooth when the stomach is over-inflated. The body of the stomach has the most pronounced mucosal folds. Even in moderate distension, they appear as long, broad mucosal ridges running in sinuous strips from fundus to pyloric antrum (Fig. 7). They are seen on all mucosal surfaces of the body but are most obvious on the anterolateral, lateral and posterolateral parts (which correspond to the inner surface of the anterior and posterior external surfaces and to the greater curvature). Here they are occasionally called the magenstrasse, a reference to their possible role in directing liquid entering the stomach immediately down into the pyloric antrum. These folds are least prominent on the medial surface (corresponding to the inner surface of the lesser curvature), which is much smoother, particularly when the stomach distends.
The areae gastricae within the antrum are small nodular elevations of the mucosal surface that are readily seen on double contrast barium meal (Fig. 7). The few folds present in the antrum when the stomach is relaxed disappear with distension. The antrum adjacent to the pyloric canal, the prepyloric antrum, has a smooth mucosal surface culminating in a slight puckering of the mucosa at the pyloric orifice caused by the contraction of the pyloric sphincter.
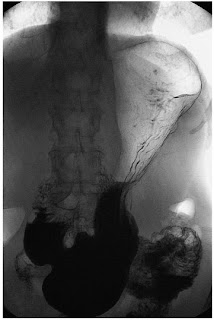 Figure 7 Double contrast barium meal in the erect position the stomach has a more 'J'-shaped configuration
Figure 7 Double contrast barium meal in the erect position the stomach has a more 'J'-shaped configuration
GASTROSTOMY
Since the lower body and antrum of the stomach is related to the posterior aspect of the left anterior abdominal wall, it may usefully be accessed to form a gastrostomy. Its mobility enables the anterior surface of the stomach to be readily approximated to the parietal peritoneum on the posterior surface of the abdominal wall and a communication to be established between the lumen of the stomach and the surface of the skin. Although this may be performed as a direct open surgical procedure under general anaesthetic it is much more commonly performed using a percutaneous puncture guided by either endoscopic visualization of the stomach or radiological imaging. The procedure is made easier by the fact that the anterior surface of the stomach lies most nearly in the vertical plane when the stomach is distended. One of the main hazards of the procedure results from the occasional interposition of the transverse colon between the stomach and anterior abdominal wall. This may lead to inadvertent transfixion of the colon by the needle puncture system. The variable length of the transverse colonic mesentery means that it may sometimes lie adjacent to the anterior gastric surface when a subject is recumbent. These risks may be reduced by radiological guidance.
Variation caused by the contents of the stomach mainly affects the body because the pyloric part usually remains contracted during digestion. As the stomach fills, it expands forwards and downwards but, when the colon or small bowel is distended, the fundus enlarges towards the liver and diaphragm. As stomach capacity increases, the pylorus is displaced to the right and the axis of the whole organ lies in a more oblique direction (Figs 5, 7). In this position the anterior and posterior surfaces tend to face forwards and backwards and the lowest part is the pyloric antrum, which extends below the umbilicus. When intestinal distension interferes with downward expansion of the body, the stomach retains a horizontal position.
 Figure 5 Axes of the empty and full stomach. As the stomach distends, the greater curvature 'rolls' downwards and the anterosuperior surface comes to lie almost completely vertical as the anterior surface.
Figure 5 Axes of the empty and full stomach. As the stomach distends, the greater curvature 'rolls' downwards and the anterosuperior surface comes to lie almost completely vertical as the anterior surface.During endoscopic examination (Fig. 6), the stomach is typically at least partially distended by air. The cardiac orifice and the lowest portion of the abdominal oesophagus viewed from above are typically closed at rest by tonic contraction of the lower oesophageal musculature. The gastric mucosa lining the orifice is puckered into ridges. It is present for a short but variable distance into the abdominal oesophagus and the transition between columnar and squamous epithelium is usually clearly visible. The presence of abnormal columnar epithelium within the anatomical oesophagus is referred to as Barrett's oesophagus but the precise definition of this condition is difficult. From within the distended stomach, the cardiac orifice appears in the medial wall of the fundus and is asymmetrical. The medial edge of the cardiac orifice is continuous with the medial wall of the body of the stomach. The mucosa is slightly thickened at this point with a raised profile, forming part of the 'mucosal rosette' that lines the orifice. The 'rosette' aids closure of the cardiac orifice and helps prevent reflux of stomach contents into the oesophagus. The medial edge of the orifice is more clearly visible than the lateral edge as it forms a more acute angle with the mucosal lining of the abdominal oesophagus.
 Figure 6 Endoscopic appearance of the stomach: A, cardiac orifice from below; B, body greater curvature; C, body lesser curvature; D, pylorus.
Figure 6 Endoscopic appearance of the stomach: A, cardiac orifice from below; B, body greater curvature; C, body lesser curvature; D, pylorus.In the partly distended stomach, the mucosa of the fundus is thrown into gentle folds with no particular pattern. As the stomach fills towards capacity, however, these folds rapidly become less pronounced, and the wall is nearly smooth when the stomach is over-inflated. The body of the stomach has the most pronounced mucosal folds. Even in moderate distension, they appear as long, broad mucosal ridges running in sinuous strips from fundus to pyloric antrum (Fig. 7). They are seen on all mucosal surfaces of the body but are most obvious on the anterolateral, lateral and posterolateral parts (which correspond to the inner surface of the anterior and posterior external surfaces and to the greater curvature). Here they are occasionally called the magenstrasse, a reference to their possible role in directing liquid entering the stomach immediately down into the pyloric antrum. These folds are least prominent on the medial surface (corresponding to the inner surface of the lesser curvature), which is much smoother, particularly when the stomach distends.
The areae gastricae within the antrum are small nodular elevations of the mucosal surface that are readily seen on double contrast barium meal (Fig. 7). The few folds present in the antrum when the stomach is relaxed disappear with distension. The antrum adjacent to the pyloric canal, the prepyloric antrum, has a smooth mucosal surface culminating in a slight puckering of the mucosa at the pyloric orifice caused by the contraction of the pyloric sphincter.
 Figure 7 Double contrast barium meal in the erect position the stomach has a more 'J'-shaped configuration
Figure 7 Double contrast barium meal in the erect position the stomach has a more 'J'-shaped configurationGASTROSTOMY
Since the lower body and antrum of the stomach is related to the posterior aspect of the left anterior abdominal wall, it may usefully be accessed to form a gastrostomy. Its mobility enables the anterior surface of the stomach to be readily approximated to the parietal peritoneum on the posterior surface of the abdominal wall and a communication to be established between the lumen of the stomach and the surface of the skin. Although this may be performed as a direct open surgical procedure under general anaesthetic it is much more commonly performed using a percutaneous puncture guided by either endoscopic visualization of the stomach or radiological imaging. The procedure is made easier by the fact that the anterior surface of the stomach lies most nearly in the vertical plane when the stomach is distended. One of the main hazards of the procedure results from the occasional interposition of the transverse colon between the stomach and anterior abdominal wall. This may lead to inadvertent transfixion of the colon by the needle puncture system. The variable length of the transverse colonic mesentery means that it may sometimes lie adjacent to the anterior gastric surface when a subject is recumbent. These risks may be reduced by radiological guidance.
To be Continued... (The Vascular, Lymphatic and Innervation)





2 comments:
I started on COPD Herbal treatment from Ultimate Health Home, the treatment worked incredibly for my lungs condition. I used the herbal treatment for almost 4 months, it reversed my COPD. My severe shortness of breath, dry cough, chest tightness gradually disappeared. Reach Ultimate Health Home via their email at ultimatehealthhome@gmail.com . I can breath much better and It feels comfortable!
I was diagnosed as HEPATITIS B carrier in 2013 with fibrosis of the
liver already present. I started on antiviral medications which
reduced the viral load initially. After a couple of years the virus
became resistant. I started on HEPATITIS B Herbal treatment from
ULTIMATE LIFE CLINIC (www.ultimatelifeclinic.com) in March, 2020. Their
treatment totally reversed the virus. I did another blood test after
the 6 months long treatment and tested negative to the virus. Amazing
treatment! This treatment is a breakthrough for all HBV carriers.
Post a Comment